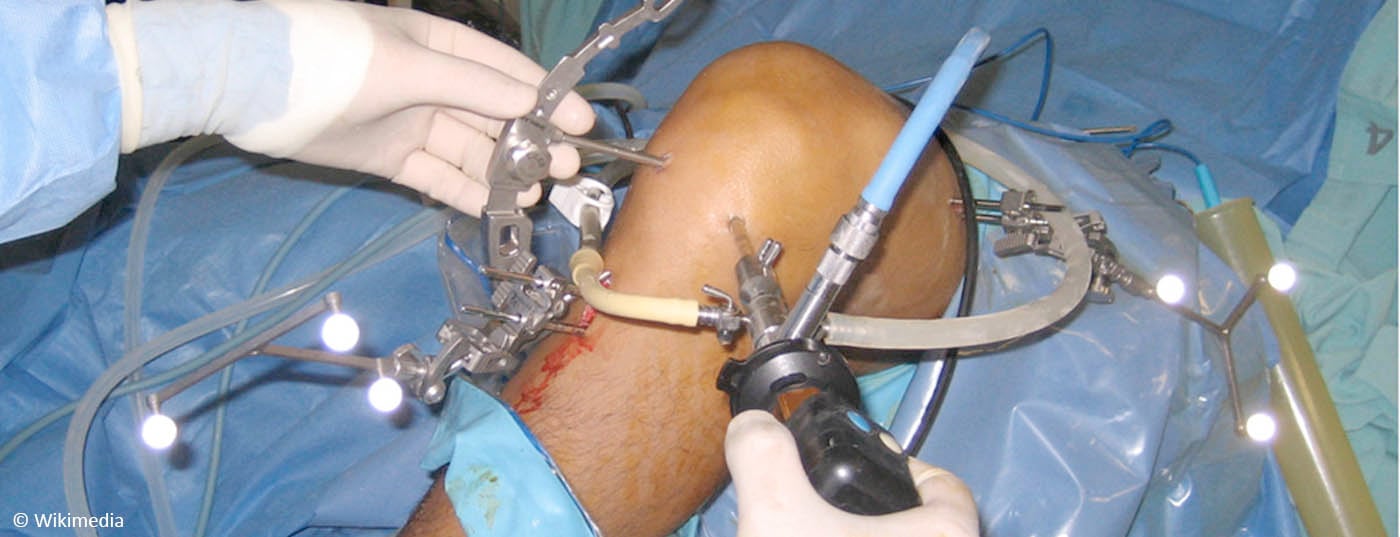
Orthopaedic surgeons practicing arthroscopy are currently facing significant challenges. From the highest echelon of the journal Olympus, a series of randomized trials have suggested that no specific treatment effect can be achieved by surgery in either cartilage damage of the knee joint [1, 2] or degenerative meniscal damage [3, 4]. Is this true? In the article, the studies in question are critically reviewed once again.
The comparative studies published in 2013 give the impression of a questionable or unproven benefit of meniscus surgery, which experience has shown to be convincing in this country when indicated appropriately. They now place the operators in a skewed light of pecuniarily motivated overproviders. As expected, the reaction of those affected has not failed to materialize [5–8]. It is gratifying to note the tone of the statements made by those affected, according to the motto: Fortiter in re, suaviter in modo (hard on the matter, pleasant in manner). These are not emotional overreactions, as one often encounters when one’s own chair is being sawn. Rather, they are carefully written analyses after in-depth study of the entire work, including the annex texts, which were not included in the main publication – probably more consciously than unconsciously – but which contain quite crucial information.
All four studies are characterized by astonishing deficiencies in the way scientific information is conveyed, especially if one analyzes the papers in full detail, has methodological knowledge of a study interpretation, and also has personal experience regarding arthroscopic surgery over decades.
Study deficiencies
Critical reading reminds one of the “Texas sniper” who first shoots a round into a wall with a pistol and then draws the target around the point of entry, simplifying the message of the “bull’s eye” [9].
For reasons of space, the above-mentioned works cannot be discussed in detail here. In the two meniscus studies, the central and decisive feature is the low prevalence of clinically relevant meniscal damage, analogous to the usual low prevalence in a family practice. It is to the credit of the general practitioners that they are able to increase the probability of a relevant meniscus injury by clinical diagnosis, assessment of the patient’s reality, the course profile and the response to conservative measures in such a way that they can offer the operating colleagues a selection of patients in need of surgery. This indication maturation is not discussed in the aforementioned studies. Therefore, the statements of the authors are not surprising.
You can compare the initial situation with a cloudy pane of glass. The cause is often a build-up of dust, which can be removed in the short term with a frond (physiotherapy, joint lavage). However, in certain cases, if a stubborn dirt sticks, sharper cleaning agents are needed (surgical intervention on the meniscus). In addition, surprisingly gross methodological blunders can be found: Discordant inclusion criteria with implications for study validity [1–4], unequal baseline of scores in run-in phase [2], fateful intention-to-treat analysis [3], high probability of score bias [1–4], hardly credible blinding [4], performing, possibly performer bias [4] and the like. In addition, it seems difficult to understand the editors’ tendency to allow scientific texts that preface the (desired) study statement and allow the limitations of the study to be discussed only afterwards, without modifying the main statement.
Questionable tactics of the editors
Connoisseurs of the scene now know that it is not enough to blindly rely on randomized studies of the highest level of evidence I even in a globally recognized, high-impact journal. As a matter of principle, randomized trials can still be used (ethics) and must be used (confounders equally distributed between both groups) if the expected outcome differences in the comparative study are small and thus clinically rather irrelevant. Thus, this study design virtually invites the design of the facility in such a way that the conclusion of no or negligible difference in outcomes can accommodate the state of interest. The NEJM tends to be run (pardon me!) by representatives of internal medicine. In the four studies, one cannot entirely deny the impression that there is a certain strategic systematicness inherent in them against an operational approach and that the lurid statements are intended to trigger widespread attention. In today’s competition among magazines, sales-related considerations are also likely to have their place in the editorial offices. In any case, it already seems to have succeeded in putting science journalists on the map and triggering TV talk shows.
Fake benefits are better recognized today
However, this is not intended to deny the need for constant critical scrutiny of one’s own professional activities in clinical studies. On the contrary, it should continue to be promoted. On the other hand, in the context of the current discussion about the sense or nonsense of meniscus surgery [5–8], it may be noted that the critical-analytical competence of the medical profession has already undergone a gratifying improvement, so that it no longer puts up with a pretense of a lacking or existing benefit, as perhaps it once did. Evidence-based medicine or clinical epidemiology provides a reliable tool to capture clinically relevant patient benefits. Thus, in diagnostic terms, the “Sherlock Holmes method” of calculating the information gain by a test and dealing with the estimation of disease probabilities [10, 11] also proves useful in promoting indication quality.
Patient-relevant outcomes
The indication for a meaningful arthroscopic intervention on the knee joint continues to be a major medical challenge, not only in the general practice, but also for the specialists.
It should always be recognizable that not knee joints but people with an individual problem are to be treated. This cannot be read off an MRI, but continues to require a meticulous collection of medical history regarding changes in abilities, a careful examination with documentation of clinically relevant findings, and an appreciation of the course profile.
Realistic expectations
From this, the realistic expectations for the best possible curative treatment method can be derived. Particularly in the case of degenerative changes in the joints in the gray zone between age-related tissue fatigue and pathological manifestation in the sense of the development of arthrosis, “repair models” analogous to a car repair shop are hardly appropriate. Rather, decisions are based on the potential for nature to cope with devitalized tissue in the joint (cartilage, meniscus), which no longer has any function and is primarily responsible for pain and painful swelling. Thus, arthroscopic cleaning aims at removing devitalized tissue to favor the conditions for subsequent (physiotherapeutic) rehabilitation.
Even if the main statements in the mentioned literature about the sense or nonsense of arthroscopic operations on the knee joint seem misleading at a high level, they might have stimulated reflection here and there.
Luzi Dubs, MD
Literature:
- Moseley JB, et al: A controlled trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med 2002; 347: 81-88.
- Kirkley A, et al: A randomised trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med 2008; 359: 1097-1107.
- Katz JN, et al: Surgery versus Physical Therapy for a Meniscal Tear and Osteoarthritis. N Engl J Med 2013; 368(18): 1675-1684.
- Sihvonen R, et al: Arthroscopic partial meniscectomy versus sham surgery for a degenerative meniscal tear N Engl J Med 2013; 368(26): 2515-2254.
- Becker R, et al: Do arthroscopy and physiotherapy have comparable results ? Orthopaedic and Trauma Surgery Communications and News, August 2013; 394-395.
- Müller-Rath R: Useless meniscus surgery? Arthroscopy 2014; 1: 70-72.
- MacDonald PB: Commentary on (1) in Evidence-based Orthopaedics. J Bone Joint Surg Am 2013; 95: 2058.
- Dubs L: Arthroscopic joint cleaning in knee osteoarthritis. Offprint from Ars Medici 2011.
- Beck-Bornholdt HP, Dubben HH: The dog that lays eggs. Rowohlt Verlag 3rd ed. 2002: 38.
- Pewsner D, et al: Tracking intuition? Bayes’ theorem and diagnostics in primary care. Praxis 2001; 3: 41-52.
- Dubs L: The decision to perform arthroscopic meniscal surgery using the “Sherlock Holmes method”. SAeZ 2003; 84(12): 541-544.
CONCLUSION FOR PRACTICE
- Remain skeptical even when publishing in high-profile journals.
- A randomized study with evidence level I does by no means mean that the statements are convincing or valid.
- The basic principle of removing devitalized tissue without function for the purpose of improving trainability may be considered reliable.
- A good indication for arthroscopic knee surgery usually also gives good results.
- Personal experience remains important, but the question of whether the good result was achieved despite or because of the treatment must always be kept in mind.
A RETENIR
- Restez également septiques par rapport aux publications dans les revues prestigieuses.
- Une étude randomisée avec un niveau de preuve de I ne signifie absolument pas que les prévisions sont convaincantes ou valides.
- Le principe de base de l’ablation du tissu dévitalisé non fonctionnel afin d’améliorer l’aptitude à l’exercice physique doit être considéré comme fiable.
- Une bonne indication pour une opération du genou sous arthroscopie donne en général également de bons résultats.
- L’expérience personnelle reste importante, cependant la question de savoir si le bon résultat a été obtenu malgré le traitement ou grâce à lui ne doit jamais être perdue de vue.
HAUSARZT PRAXIS 2014; 9(4): 22-24