Urogynecology and reconstructive pelvic floor surgery are in a phase of upheaval: the ban on transvaginal polypropylene mesh kits in many countries has fundamentally changed the surgical strategy and provided new impetus for native tissue repair techniques and minimally invasive approaches. At the same time, the AUA/SUFU Guideline 2024 has restructured the management of overactive bladder – moving away from rigid staged regimens towards patient-centered treatment choices. Robotic sacrocolpopexy is establishing itself as the standard for apical defects, and new findings on de novo stress incontinence after prolapse repair are influencing preoperative counseling.
Publikation
- GYNÄKOLOGIE PRAXIS
Related Topics
You May Also Like
- New evidence on descensus, urinary incontinence and the future of reconstruction
Urogynecology and pelvic floor surgery 2026
- Proteins in wound healing
Do special amino acids lead to success?
- Case study
Autosomal recessive polycystic kidney disease: atypical phenotype
- Current evidence, risk classes and new counseling options
Hormonal contraception and cardiovascular risk
- Acute otitis media: self-limiting course vs. "red flags"
In which cases are antibiotics necessary?
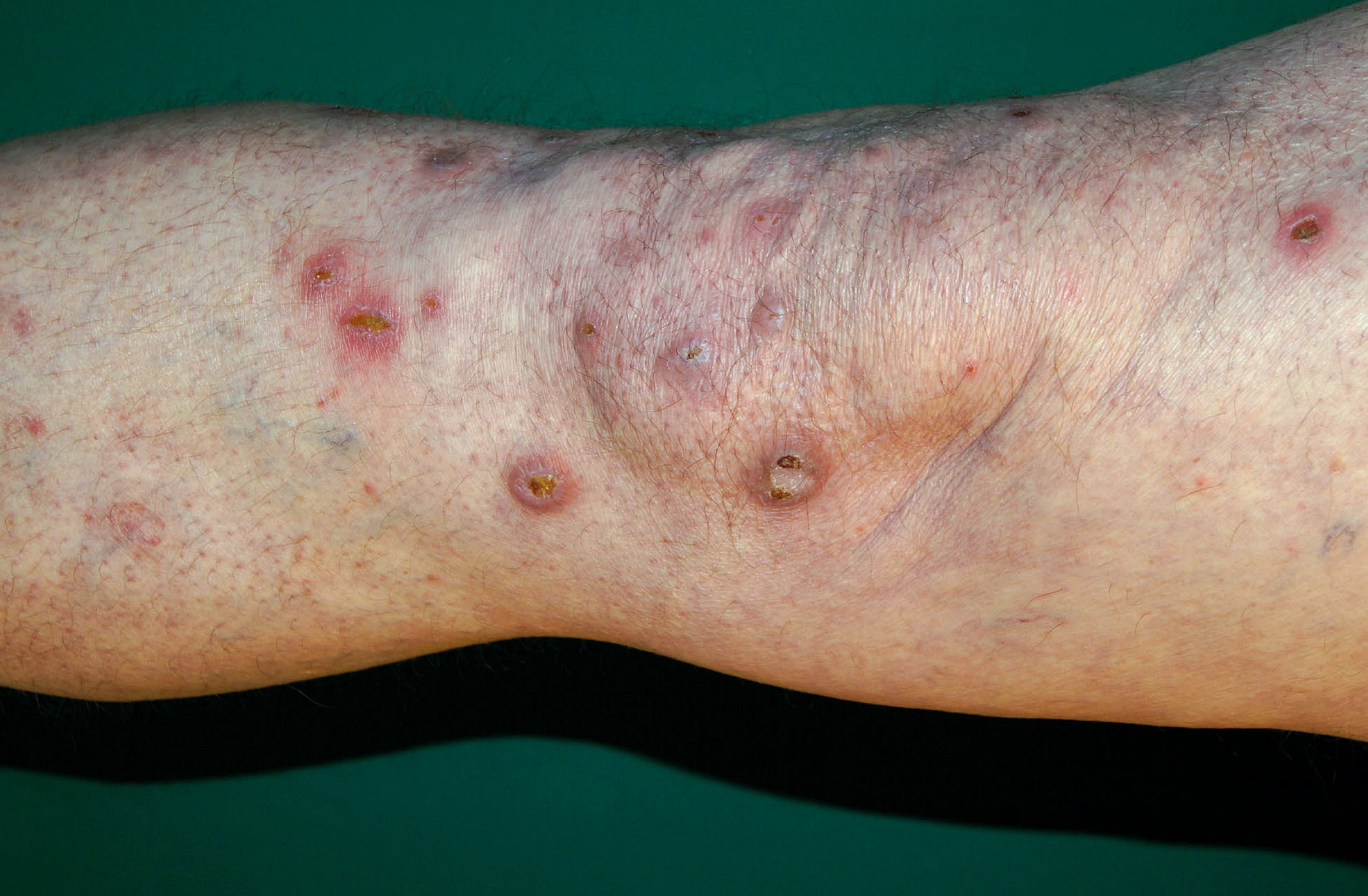
- Prurigo nodularis: evidence-based treatment
Targeted therapy options on the rise
- MACE risk, heart failure incidence and all-cause mortality
Metabolic syndrome as a cardiovascular risk factor
- Glaucoma in old age: slowing down progression